When it comes to mental health services, an enormous gap exists within our healthcare systems. Employees are getting more sick, and there aren’t enough face-to-face therapists to meet the demand. As leaders, we know that our employees’ mental health is important and critical to the success of our businesses as we recover from the economic impacts of COVID-19. We also know that critical barriers prevent them and their families from accessing the help they need, including cost, wait times, and stigma.
Innovative and creative delivery models are becoming essential to improving access to affordable, immediate, and effective mental health support that meets each individual’s unique circumstances.
Today, the proposed approach is called the “Stepped Care Model”, coined in the UK and adopted by other countries, including Australia, the United States, and Canada.
But what is Stepped Care?
Stepped Care 1.0 is the original UK stepped care model. It’s commonly known as a system for assessing, delivering and monitoring mental health treatment so that the most effective and least resource-intensive treatment is delivered first, before a more intensive, specialized service is needed. Simply put, the Stepped Care model focuses on linking a person with the right level of support to avoiding under-treating or over-treating them.
Today, Stepped Care has evolved to a 2.0 version. The new version integrates a more flexible, client-centric approach, combining a range of traditional and emerging digital mental health interventions to systematically determine care options for individuals at the right time, with the right therapy, in the right context, focusing on triaging individuals based on therapy history, condition, preferences, functioning, and readiness to engage with therapy, instead of only the diagnosis or symptom severity.
The advantage of the stepped care model is that it maximizes the effectiveness and efficiency of support by optimizing resource allocation.
The following figure details a standard stepped care model for mental health support.
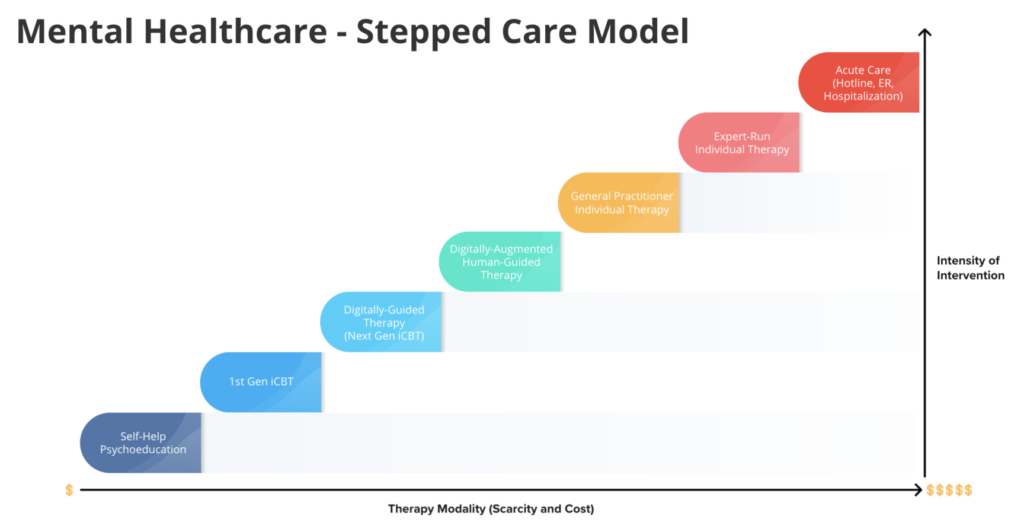
- Step 1: Uses interactive self-help resources, such as workbooks or courses for online application. These tools can be helpful for individuals who may not be ready or have the need, to engage in therapy fully but are willing to explore what might be involved in making small changes.
- Step 2: 1st generation iCBT take a linear approach to CBT and is available through EAPs for basic mental health support. These tools can be helpful for individuals who would like to better understand their mental health and how to manage it
- Step 3: 2nd generation iCBT take a personalized, patient-centric approach to iCBT to deliver highly engaging, scalable mental health therapy that emulates human-guided therapy
- Step 4: Digitally-augmented inventions include an interactive blend of digitally-guided and human-guided therapy to personalize support for an individual
- Step 5: Involves one-on-one counselling sessions through a general practitioner, though they may not have the expertise or training to help someone with more complex needs
- Step 6: Involves more intensive one-on-one counselling sessions through a specifically-trained human-guided therapist, psychologist, or psychiatrist to deliver expertly run sessions
- Step 7: Involves intensive case management and crisis support for individuals with chronic conditions, substance use or severe behavioural issues. This includes more intensive services such as admission to a hospital psychiatric ward
Our healthcare systems that rely on human-guided therapy (i.e. face-to-face, teletherapy) are becoming unsustainable for today’s mental health demands and will likely intensify in the aftermath of the COVID-19 pandemic.
Today, many organizations have an EAP or EFAP in place and often layer on face-to-face therapy alongside an iCBT offering to deliver support in Step 2, alongside two to three sessions in Step 5 or 6. EAPs can be a powerful resource when properly utilized though the benefits are often not realized due to the limited benefits, low engagement rates, and stigma surrounding the offering.
Only large enterprise companies offer psychological benefits available in Step 6 through their group health insurance plan, mainly due to it being an expensive benefit ($2500 – $5000), further hindering someone’s ability to access mental health support.
The stepped care model 2.0 is intended to utilize digital interventions to provide more affordable and scalable access to therapy in a healthcare system riddled with chronic shortages of qualified health professionals and disparities in access due to cost, difficulty finding services, geographical limitations, and stigma.
The stepped care approach has four core elements:
- Assessments: Segmenting the population into different groups based on needs, condition & severity, therapy history, personality
- Service Types: Developing and defining each stepped care option into seven or more steps
- Interventions: Delivering a comprehensive system of informal and formal evidence-based services
- Personalization: Matching service types to the treatment needs of each group segment
Assessments
Assessments for mental health patients are usually done by their General Practitioners (GPs) or mental health professionals. GPs are generalists and often lack the adequate training to accurately assess and diagnose an individual, and mental health professionals are costly, especially if multiple assessments are needed. An hour evaluation with a mental health professional could run between $124 – $188 USD, although a full assessment can run up to $1500 – $3000 USD. This creates a problem within stepped care as the model currently lacks a centralized system to monitor whether or not an individual needs more or less intensive therapy levels. There needs to be an assessment tool that is accurate, scalable, and cost-effective in flagging any individuals at the wrong level of mental health support and routing them to the right level of care.
Assessments in our current culture also tend to focus on identifying the diagnosis instead of an individual’s therapy preferences and functioning, leading to them misplaced in the stepped care model. Assessments, check-ups, and intake screeners must take a broader approach and consideration for an individual’s therapy history, preferences, personality type, readiness to get help, and overall functioning to ensure they get the therapy most suited to them as quickly as possible. This is to increase the likelihood of them continuing with their therapy. A bad experience at one level for too long could discourage someone from seeking care, further emphasizing the need for accurate, comprehensive intake screeners and assessments. Regular check-ups will also help determine if the individual should be moved to another level suitable for their current emotional and mental health. This will help ensure therapy continuously adapts to the needs of an individual and prevents the system from undertreating or overtreating them.
Service Types and Interventions
When considering the best approach to mental health, there is general agreement among health, public health, and health plan providers that prevention and early intervention must be prioritized within the stepped care model to prevent worse-off physical and mental health outcomes. As such, a full spectrum of prevention and early intervention options delivered both digitally-guided or human-guided must be available to cover a wide range of different personality types, preferences, or individual circumstances.
For instance, due to exhibiting mild or moderate anxiety symptoms, an individual is initially assessed and routed to a digital CBT platform like Starling Minds. However, our regular assessments and checkups determine they need more intensive human-guided therapy due to additional life stressors. Therefore, they are immediately flagged and re-routed to ensure they are getting the right level of support. Stepped care works best when healthcare providers work collaboratively to deliver the right level of care to members, whether it’s digital therapy for mild to moderate conditions or human-guided therapy for severe cases.
Starling’s full-spectrum, digital therapy platform includes two solutions:
- Starling Minds Mental Fitness: An early-intervention Cognitive Behavioural Therapy (CBT) program that personalizes digital therapy to address stress, anxiety, and depression of healthcare and education workers
- Starling Minds Return-to-Health: A return-to-work CBT program that supports rehabilitation and provides workers with the skills and confidence to integrate back into work, whether they are on a physical or mental health claim
During therapy, digital options can also provide consistent and quality support that emulates human-guided therapy by having therapy recommendations served up by our Expert System to the “generalist” therapists in Step 5.
Personalization
The heart of stepped care is to effectively match the service type to the therapy needs of an individual. Today, face-to-face therapy still receives the highest efficacy results due to a psychologist or psychiatrist’s ability to adapt their sessions to each individual. However, as trained, experienced mental health professionals begin to retire, there will be a significant gap in highly qualified experts due to fewer people entering the field. COVID-19 has also added more burden on our overextended systems, including telehealth. As a result, digital interventions have been brought to the forefront and challenged to emulate the practices of human-guided therapy, but without the barriers associated with face-to-face, like cost, access, and stigma.
In conclusion, Stepped Care Model 2.0 has gained a lot of momentum over the last few years. However, the system will not be sustainable without its core elements to deliver the right therapy, to the right patient, in the right context.
To learn how Starling can help you deliver the digital interventions of the stepped care model, reach out to us.




